Hip Impingement and Labral Tears
Have you been diagnosed with hip impingement? Maybe a labral tear?
have you Been told that surgery is the only option to correct this?
While hip impingement is painful and frustrating, it is not a condition that needs to be scary. It is not a dead end road and a sentence for chronic pain. It does not REQUIRE surgery.
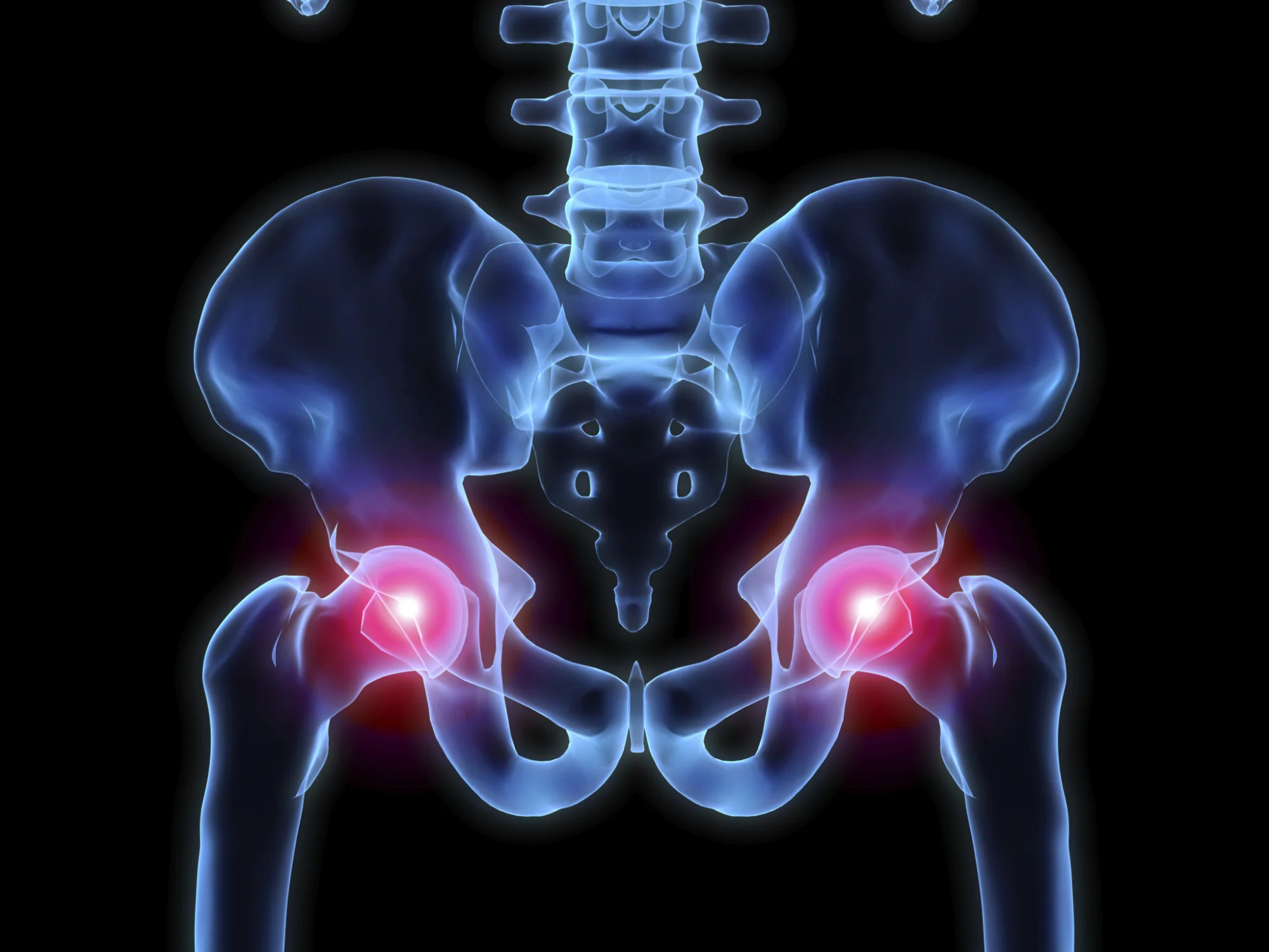
Impingement is the word used to describe a painful contact between two surfaces, which often causes pain. In the hip, this can be anatomical or functional. Anatomical impingement involves bony abnormalities interfering with joint movement. If the symptoms of impingement are present without the bony abnormalities, this is called functional impingement.
These are images showing the different presentation of the bony abnormalities associated with anatomical impingement.
symptoms of hip impingement can include:
stiffness or deep aching in thigh, groin or hip
sharp pain in the groin or buttock when the thigh is moved close to or across the body
pain with sitting for long periods
difficulty with weight bearing
clunking, popping or clicking of the hip
pain at rest and/or with activity
pain during and/or after sexual activity
pain during or after sports
low back, sacroiliac joint, or knee pain
BOTH ANATOMICAL AND FUNCTIONAL HIP IMPINGEMENT RESPOND WELL TO PHYSICAL THERAPY INTERVENTION.
Restoring motion, improving muscle balance, and returning a patient to more correct movement mechanics and motor patterns are all key in this care. Patient education about correct rehabilitation exercises and stretches as well as managing outcome expectations are also included in the care of the hip impingement patient.
More and more evidence is coming forth demonstrating that the surgical outcomes to correct hip impingement and labral tears are not any better than physical therapy. In many cases, because a patient is promised relief and full function following surgery, the outcomes actually point toward increased depression and chronic pain when the surgery does not lead to relief. However, sometimes surgery is indicated and can help the correct patient. This further emphasizes the importance of a comprehensive evaluation and treatment plan to put you on the right path to relief.
We are different at Arrow Physical Therapy Seattle!!
Sarah speaking to physical therapists on what we need to be doing differently with our patients suffering with hip impingement and labral tears.
We will always support our patients in their medical journey but feel that they deserve honest and clear conversations even if they are not easy to have. We believe that there is so much we can do outside of surgery but we do know that our treatments are different here. If you have tried physical therapy for your hip pain and are still hurting, please reach out. We are here to help YOU.
We have lots of resources on this topic:
BLOG ARTICLES
VIDEOS
HOME PROGRAMS
Check out this e-book for more information!!
Limited range of motion? Throbbing and aching? Difficulty with daily movement and sport? Minimal relief with stretching and now avoiding the things you love? You may have hip impingement. If you have you been searching for a non-surgical solution and tried physical therapy without success, HIP FIX is for you. This step-by-step digital guide will teach you how to strengthen and change the way you move so that you can return to a pain-free life. Change how you move. Change how you feel.